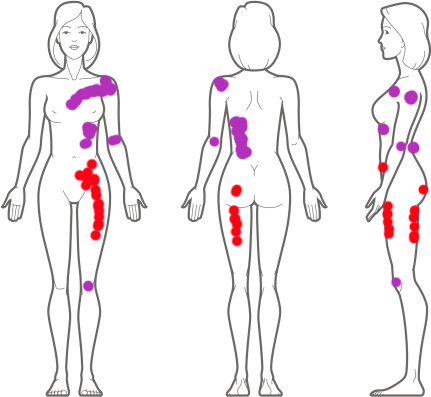
Everywhere I experience chronic pain. Endometriosis in red and JHS in purple.
Earlier this month I got a letter from a rheumatologist confirming that I had Joint Hypermobility Syndrome (JHS). This is the second long term condition diagnosis that I’ve received. My first was my diagnosis for endometriosis in 2009.
It didn’t really come to a surprise for me to discover I had another long term condition, because I’d been experiencing pain that didn’t quite tally with endometriosis for quite some time (almost two years). However it was getting worse and I didn’t know how best to manage this new type of pain.
Not everyone with one long condition will go on to develop a second or third, but some of us do, and I know what you’re thinking, “I can’t manage with one long term condition, how could I manage with two?”.
It’s rather like your first diagnosis to be honest – you don’t have a lot of choice in the matter.
What is joint hyper mobility syndrome?
Joint hypermobility means that some of my joints are more flexible and move more than they should. This isn’t necessarily a problem (it’s known colloquially as double jointedness). It becomes joint hyper mobility syndrome when you have significant, long term pain and other problems caused by the joint pain and if you have a high Beighton score. In order to be diagnosed my symptoms and location of my pains were noted and then I was examined. I completed the Beighton test, scoring 8/9.
This involves tests like, being able to bend your little fingers back quite a way. Being able to bend your thumb forwards to touch your arm, and being able to touch the floor with your palms when your legs are straight and together. Here’s some more detail on the beighton test if you’re interested.
Following this, the Brighton score is used to indicate likelihood of joint hyper mobility syndrome, and lucky me, I win the prize.
Will I be changing my website?
No. Many of you that read don’t have endometriosis, and you’ve told me that you’ve found the information I’ve given on living with chronic pain and fatigue as useful for your condition as it is for endometriosis. So I will keep going under the current name.
If anything getting a second diagnosis has given me great insight into how endometriosis diagnosis compares with another condition. I’ve come to realise that other conditions can have much better care pathways when compared to endometriosis. So I still have a lot of work left to do.
From what I can see online endometriosis and joint hyper mobility syndrome have a good crossover with an above average number of women experiencing both. It’s an area I hope to research more. I am particularly interested if both conditions are in all likelihood something that I was born with that “decided to show up” later in life or if JHS would have appeared without endometriosis. I can’t help but wonder, did my treatment for one instigate this pain in some way?
I still have a lot of questions.
Only this time around I feel confident asking more questions, and I’m able to communicate with my specialist more (mainly because I have two people to talk to rather than just one).
I’ve been here before…
First time around I remember the relief of finding out the pain I was experiencing had a name. That it was common wouldn’t threaten my life and could be treated. My life with endometriosis would be okay. Only it hasn’t been as straight forward as that.
Back when I first got my diagnosis I had a different sort of hope. I felt cared for by the people treating me it felt like if the help was always like this it would be ok.
Several years later (when that professional help has moved away). I have a more realistic perspective on the situation. I analyse the information I am given so much more. I’m doubtful of bold statements about how my health should improve with certain treatments because I’m so aware of how complex living with conditions like endometriosis can be. Treatments have side effects, and they take a long time to start giving you relief.
I’ve been through the process once before and I can benefit from that experience. I’m not racing “to get better” because in reality the improvement will take longer than my dash to the finish line. In short, the second illness has been easier to wrap my head around than the first one.
This is part of why I’ve been so quiet of late, I’m been trying to adjust under this new set of circumstances. This additional new (and terrible) level of pain is taking a long time to get used to. What helps endometriosis doesn’t help my other type of pain and vice versa. I’ve been waiting for various hospital appointments, scans, consultant appointments, as well as lung and heart tests. We’re still not quite to the bottom of why my chest hurts so much all the time and why it’s hard for me to breathe.
In the meantime I’ve had to rule out endometriosis moving to my diaphragm, problems with my lungs, problems with my heart and other long term illnesses such as arthritis and fibromyalgia.
Despite the myriad of tests I remain fairly stoic. I want what all people with chronic illness wants – answers to the questions that keep us up at night. I may not get all the answers I want. There’s a chance that the presence of JMS might be a happy coincidence. It’s certainly something I’ve lived with my whole life happily up until now, perhaps it’s just something that’s decided to reveal itself and cause me problems now.
Sadly second diagnoses can be common
I don’t wish to scare anyone, but I’m not alone in having more than one condition. There are plenty of people out there in the chronic health community with more than one physical or mental health problem. Doctors call this comorbidity. Having certain illnesses can increase your chances for developing another illness. It’s not a guarantee though and like everything with chronic pain, everyone is different and walks their own paths. Many people manage with one illness and many more find a way to manage with two or more.
So, where does it hurt?
The hardest thing about having two physical illnesses is that it’s really hard to tease apart the symptoms. Things aren’t black and white anymore. If I feel pain I’m not always certain if it’s endometriosis or joint hyper mobility syndrome. If a doctor asks me if I have bowel problems I can say that I do but I’m not sure if the endometriosis or JHS causes or exacerbates it, because they both can. It’s also really hard to know when my chronic fatigue is caused by my endometriosis, JHS or both.
I can tease apart about 70% of the pain symptoms from one another, although they’re so closely woven. My endometriosis pain makes my left hip pelvis, leg and back all spasm, in short, startling stabs of pain. The hyper mobility pain manifests in stabbing aches in my left shoulder and elbow. That much I am certain of.
However I don’t know if JHS causes the immense pressure on the top of my ribcage, the constant “squeezing” on what feels like the bottom of my left lung. It feels as though my lungs and chest are being controlled by someone other than me, a masochist puppet master that makes my heart race when I rest and makes my attempts to breath in and out something I am keenly aware of, every minute of every day. Even when I am resting, comfortable and happy. We breathe more than 17,000 times a day and I feel each breath. All the time.
My pain landscape has totally changed, my body is unknown to me again, but slowly I am re learning my new normal. I’m awaiting physio to help me with my pain symptoms. It remains to be seen if it will help my breathing difficulty. I live as normally as I can until I know otherwise.
Life is still good, but the getting the pain to be quiet has become harder. People don’t know how we can manage with one pain, let alone two, but… you find a way. 😉
Hi, thank you for writing even though it must feel rotten. Your blog is really helpful, thank you. Wishing you all the best.
Thank you so much – still got tons of ideas for things to write just need the energy and time now 🙂
I sadly can relate. 8 months after my partial hysterectomy and last excision for endo I developed two conditions that involve vertigo. One I already had and vertigo was an added symptom (migraine) the other was new. The creation/exacerbation of both is believed to be in large part to stress on my body when being treated for endo and the constant hormone changes since I was on BC, Lupron, then BC again, and Visanne back to back in less than a year. We’re learning more and more about how trauma to the mind and/or body can lead to the emergence of chronic health problems and/or cause those health problems to develop earlier in life. I’m sorry you’re going through this too.
Regarding illnesses with similar symptoms with my Migraine Associated Vertigo and Meniere’s Disease (inner ear disease that involves vertigo) with time I was able to tease the two apart. It was empowering and took a lot of self observation and patience. It will hopefully get to that point for you with hypermobility and endo.
Wishing you the best from a fellow endo sister.
Hi Michelle-
I too have a secondary diagnosis of chronic lyme disease. I agree with you that it is very often difficult to tease out one from the other. And it is also difficult to have two syndromes that aren’t well understood or even accepted in the medical community at large. It so often leaves me feeling confused and concerned that much of it is “all in my head”. Fortunately I have a physician who believes that I have all of these random aches and pains, and I certainly know I do. I appreciate your blog and know that others are facing similar challenges. I hope that you are well enough to continue. Take good care of yourself.
My Best-
Aimee
Thank you Aimee, I have no plans to stop, just finding I have to go a bit slower when it comes to writing 🙂
Hi Michelle,
So sorry to hear about your diagnosis. I found your blog deeply comforting when I was diagnosed with Endo. Sending you lots of love and best wishes. x
Thank you so much – still finding my feet but I’ll find a way. More updates to come soon.
Hi Michelle,
I wanted to thank you for putting this out in public. I have been dealing with chronic pelvic pain for close to 10 months all together. Now, I’m 2 days pre-lap to see if I have endo, and I just wanted to say thank you for giving me hope.
Hi Amanda, I hope your lap went okay, and that you’re coping well with your diagnosis (if you have one). It’s not as simple as “it gets easier” because it doesn’t necessarily, you just get used to the idea and you’re not as shocked about it over time. Good luck!
Hey, We met at a conference some years ago and you were going through an upbeat time with endo and I was going through a hard time.. I was walking with a stick.. I have gone on to have 2 children :@) But I am now being investigated for a second condition. Thank you for your blog x
Oh me oh my… bless you.
Unfortunatley i know exactly how you are feeling… 4 years ago, prior to having kids i was undergoing, exacminations for endo… then i fell pregnant and it all got put to a holt, now 4 years later, two cesareans later and I still havent booked that doctors appointment to get a diagnosis. And its worse, way way worse than its ever been… Im afraid of going back as i dont want to have to go from the start again “here try the pill, see if that helps” and ” oh that didnt work, well try some IBS tablets” or “oh well i suppose now we need to look more gyenologiclaly at you”- eugh!!! Give me strength! I also have JHS…. diagnosed, but i live and work with it. Im leaning on htese posts a little bit, to give me the strength to get be back in my doctors chair.
Stay safe kiddo,
Your doing great!
Thanks for sharing your story, it’s nice to hear about someone else with similar complications. I hope you get some progress with an endometriosis diagnosis if you decide to continue down this route.
I must say I was surprised when I found your blog after I did this search on the internet – “Is there a connection between endometriosis and hyper mobility syndrom”. I am a woman, 51 years old. I have been suffering endometriosis since I was 14. I did not get diagnosed until I was 45, and sent directly to the operating table. I have always had discomfort in my joints, but it accelerated after I reached menopause. I was diagnosed with hyper mobility syndrom last summer, and a lot of pieces in the puzzle fell into place. My biggest problem however, is FATIGUE!!! After years and years coping with pain, I have not got any excess energy left in my body. I wish there was somewhere I could get some help, but in my experience, health personel seldom understand, or know what to do. It is comforting to know that there are other people out there with the same symptoms as I have.
A big hug from Karen in Norway
Thanks for sharing Karen, nice to know I am not the only one.
Thank- you for the story is much appreciated. I can relate to most of everything you have gone thru. I been dealing with it for about 4 years. I just been learning to deal with the pain and read my body for triggers. I know sometimes it seems like never ending pain and that no one understands but we are all around and we understand the pain. We just have to keep informed of new ways to fight the good fight. I send you and everyone reading your story GOOD VIBES ALLWAYS!!!
Funnily (but not funnily) enough I got diagnosed the other way around – diagnosed with JHS about a year before being diagnosed with endometriosis. I also have IBS or some currently undiagnosed gut and stomach problem. I completely get what you mean about them blurring in to each other though. It’s hard enough when you just have one illness that flares up but when they all flare up and all cause each other to flare up it becomes such a confusing mess?! I’ve spent the last few days feel pretty awful and achy and feverish but for the life of me don’t know what’s flaring up or what the problem is, quoting parks and rec it’s just ‘everything hurts and I’m dying’ 😂
Thanks for this website though, it’s reasuring but sad to know others are going through similar things x
This is crazy… I had no idea that it was common to have JHS and endometriosis at the same time. I have JHS and suspect I have endometriosis as well. I have an ultrasound for the diagnostic process tomorrow and I’m so nervous. I don’t want to have 3 diseases, but I feel the same way as you: if I do, at least I will have some answers and hope of being treated.